Skin Cancer Symptoms
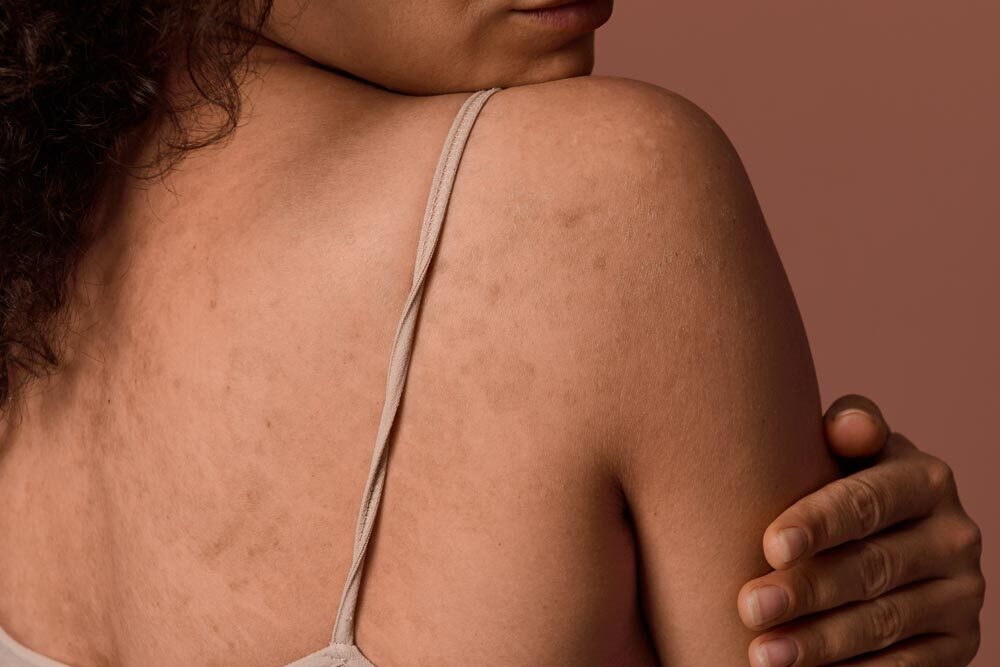
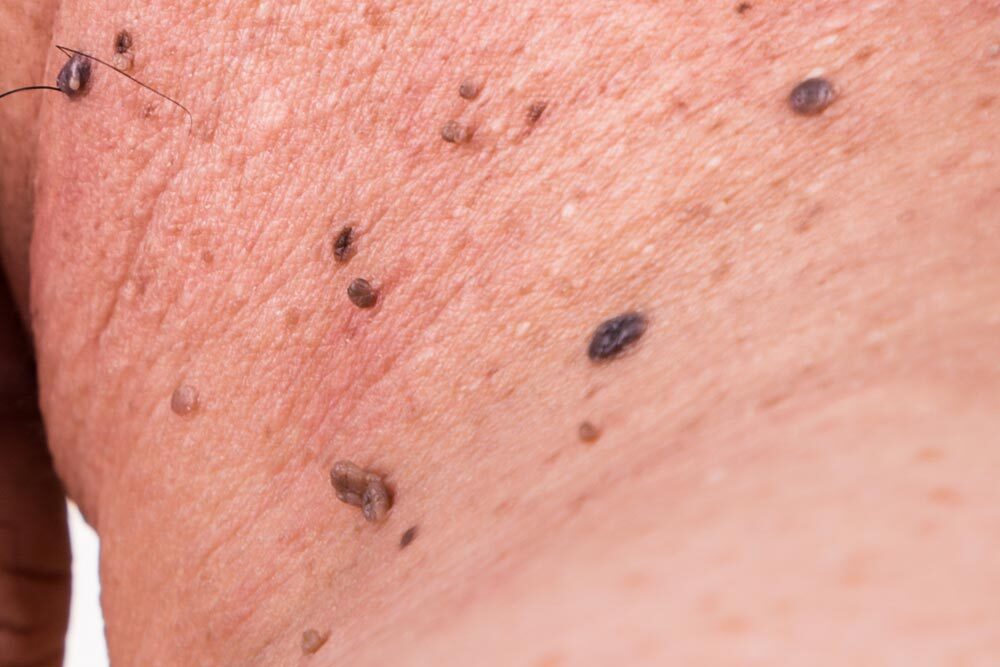
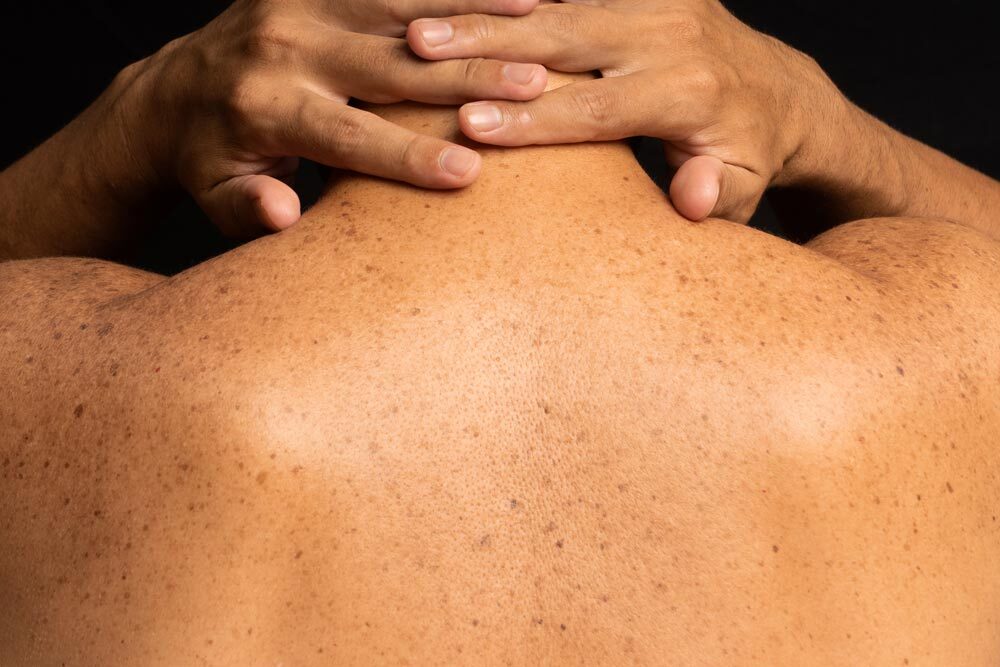
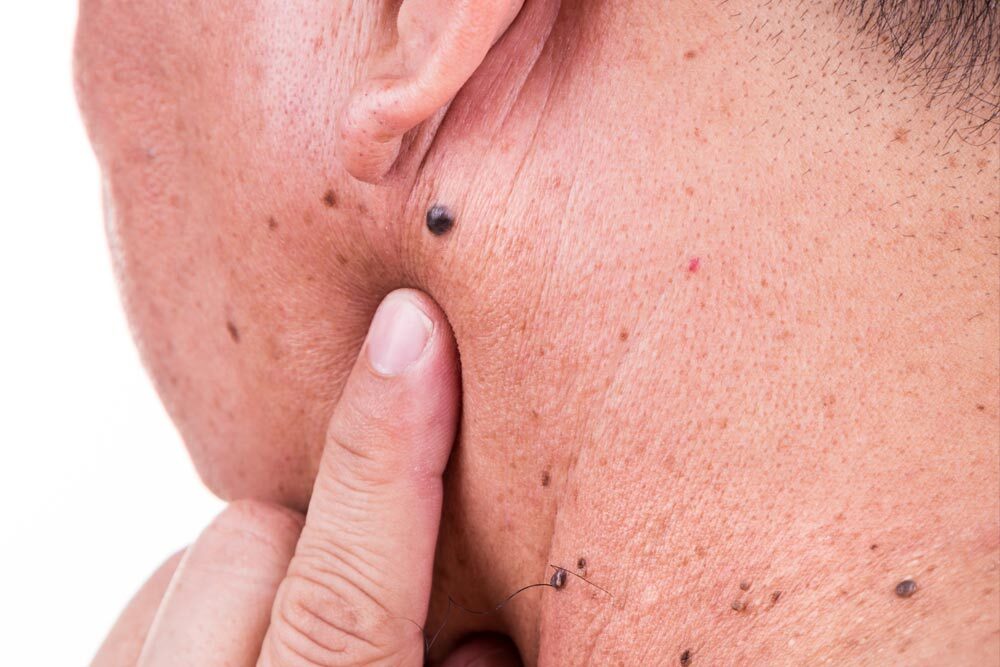
![]() The most critical warning sign of skin cancer is the appearance of a new spot on the skin or changes in an existing spot that seem abnormal. Following the A B C D E guidelines can help you identify the common signs of skin cancer:
The most critical warning sign of skin cancer is the appearance of a new spot on the skin or changes in an existing spot that seem abnormal. Following the A B C D E guidelines can help you identify the common signs of skin cancer:
- Asymmetry:One half of a mole (or birthmark) does not match the other half.
- Border:Edges are irregular, ragged, notched, or blurred.
- Color:The color is uneven, often featuring different shades of brown or black, along with patches of pink, red, white, or blue.
- Diameter:The spot is larger than 6 millimeters across (about the size of a pencil eraser).
- Evolving:The mole is changing in size, shape, color, or elevation.